Sleep apnea is a prevalent respiratory problem, affecting between 10 and 30 percent of the population. Positive airway pressure (PAP) is one of the most frequent therapies for sleep apnea. Although continuous positive airway pressure (CPAP) is the most widely used PAP therapy, bilevel positive airway pressure (BiPAP or BPAP) may be more effective for some patients.
Although the two types of PAP therapy accomplish comparable ends, there are important distinctions between them that should be taken into account. You should always consult with your healthcare provider before making a change to your PAP therapy.
How Do BiPAP Machines Differ from CPAP Devices?
In most cases, CPAP devices may be adjusted to produce air pressure anywhere from 4 to 20 cm H2O (centimeters of water pressure), regardless of whether the user is breathing in or out. A typical range is 8–10 cm H2O. CPAP machines traditionally only have one pressure setting; however, some newer models include a pressure relief feature that reduces the force of the air during exhalation.
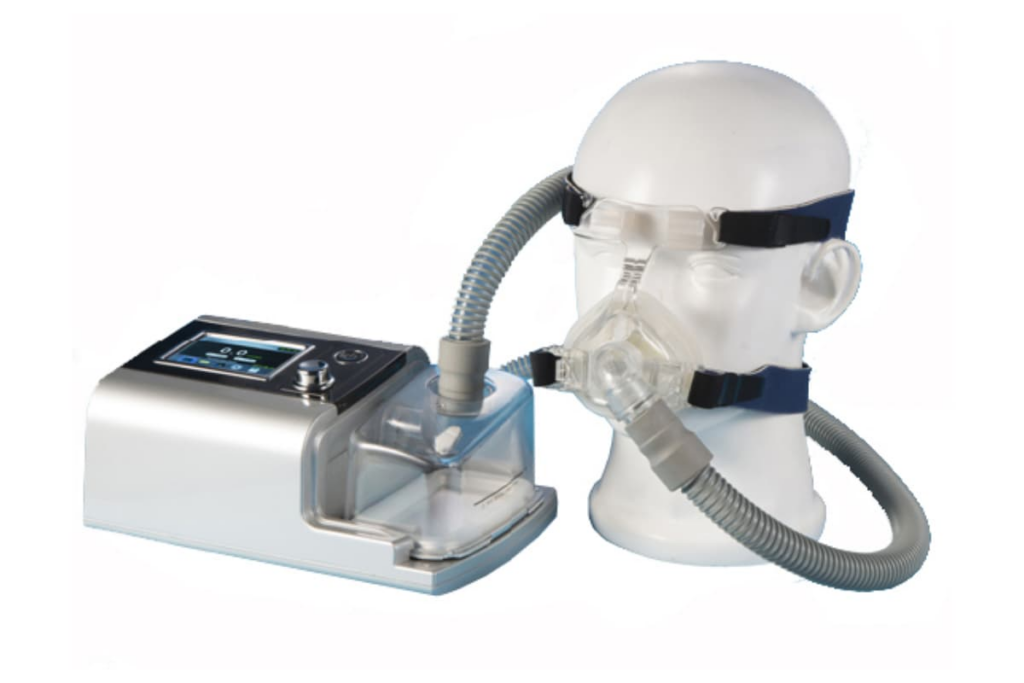
Both continuous positive airway pressure (CPAP) and bilevel positive airway pressure (BiPAP) machines are examples of positive airway pressure therapy, which employs the use of compressed air to open and support the upper airway while sleeping. The compressed air is produced by a portable machine and delivered to the user’s airway via a hose and mask. The masks, hoses, and other components of both systems are virtually interchangeable.
Related: Can EPAP Replace CPAP?
Bilevel positive airway pressure (BiPAP) machines have a lower pressure setting for exhalation, called exhalation positive airway pressure (EPAP), in addition to a higher pressure setting for inhalation. The BiPAP machine can be programmed to automatically or manually transition between IPAP and EPAP at defined intervals or in response to the user’s breathing patterns, respectively. Most bi-level air pressure (BiPAP) machines have pressure settings between 4 and 30 cm H2O.
Polysomnography, or an overnight sleep study, is required to find the optimal settings for both BiPAP and CPAP.
In contrast to BiPAP machines, which are intended for usage in the home, portable CPAP devices are ideal for travel. Compared to a similarly featured CPAP machine, the price of a BiPAP machine is typically higher due to the need for additional sensors and settings.
Although there is some crossover in the efficacy of PAP therapies, certain kinds tend to function better for different conditions. Sleep doctors are reluctant to prescribe BiPAP to patients with OSA unless they have tried and failed to respond to CPAP therapy for OSA.
Some insurance companies will pay for either CPAP or BiPAP if you have OSA, but those that do typically want proof that CPAP treatment is ineffective or intolerable before they’ll pay for BiPAP equipment. Central sleep apnea (CSA) and other conditions requiring a constant flow of air to keep the airway open while sleeping are the most common indications for BiPAP therapy.
There is a wide selection of accessories, both built-in and after-market, for CPAP and BiPAP machines. Typical examples include humidifiers and heated tubing for climate management, as well as data collection capabilities. Here’s a table comparing BiPAP and CPAP machines;

How CPAP Machines Work
While the user sleeps, a CPAP machine forces compressed air into their airway at a pressure of between 4 and 20 cm H2O. The user’s airways are kept open and they are able to breathe normally thanks to this pressure, which is the primary symptom of sleep apnea.
The inability to exhale normally or the sensation of choking may occur in some users because CPAP machines continuously pump air at one pressure setting rather than fluctuating in pressure between the inhale and the exhale. While the majority of patients adapt well to CPAP, others prefer BiPAP.
It’s important to note that CPAP machines come in a wider variety of sizes than BiPAP machines. The standard home usage model is around the size of a shoebox, whereas portable models may fit in the palm of your hand. Some FAA-approved devices are available for use on airplanes, while travel variants may include backup batteries for use while camping.
What you Need to Know About BiPAP Machines
The intake (IPAP) and exhalation (EPAP) air pressures of bilevel positive airway pressure machines can be adjusted independently (EPAP). It is common for the EPAP setting to be substantially less intense than the IPAP setting, allowing the user to exhale more naturally and with less of a sense of struggle. BiPAP machines typically have a pressure adjustment range of between 4 and 30 cm H2O.

Up to three IPAP/EPAP settings are available on most BiPAP machines.
Automatic: The user’s breathing pattern is detected, and the pressure is switched between the two settings automatically when the user inhales and exhales. This is the default for BiPAP machines and is used by the vast majority of patients.
Using timed switching: Here patients can set the duration of both the IPAP and EPAP phases to their liking. This works similarly to a ventilator in that it ensures the user is taking the proper number of breaths per minute.
Automatic and Timed: This mode is mostly spontaneous, responding to the user’s breathing patterns, but it also includes a timed component. When this option is selected, timed switching activates when the device detects that the user’s breathing rate has fallen below the specified threshold.
BiPAP machines also come in two different varieties: stationary and auto-adjusting.
A fixed BiPAP machine has IPAP and EPAP settings that do not alter during the night.
Auto-adjusting BiPAP machines allow the user to specify a range for both IPAP and EPAP. Because of this, the device may adapt automatically throughout the night based on the sleeper’s breathing patterns.
Which Is Better for You: CPAP or BiPAP?
You should know that there are important distinctions between CPAP and BiPAP machines, despite their superficial similarities. This means you should always consult your medical staff before making a change.
There is typically an acclimation phase for CPAP users before they become fully comfortable with their devices. Setting changes, trying out alternative climate control accessories like masks, or utilizing a machine that slightly reduces air pressure on the exhale can all help alleviate discomfort. If a patient is having trouble with CPAP therapy, they may be able to move to BiPAP treatment, but this is something that has to be discussed with and monitored by a sleep doctor.

